Colten Care granted planning consent in Bursledon following HPC support
Following recommendation from national planning consultants, HPC was approached by established regional care operator Colten Care in March 2025 in order to advise upon Care Home Need Assessment.
More
HPC provides Care Home Need evidence in Oxfordshire at Appeal Inquiry
As South Oxfordshire tinker with the Local Plan, this Inquiry secured outline planning consent for both residential and care home use on the outskirts of Oxford.
More
HPC Acquires Prime Site for Angela Swift Developments Group
HPC have acted on behalf of Angela Swift Developments Group Ltd in the acquisition of a former convent and grounds in the affluent and leafy residential area of Worsley, Greater Manchester.
More
Residential Care Service for Sale - West Yorkshire
Established and highly profitable with 68 beds and management in place
More
Planning Success in Horsham
HPC provided vital Care Home Need analysis in support of this care home redevelopment
More
HPC Acts in Transfer of Purpose Built Derbyshire Care Home
HPC has acted on behalf of an established client in the transfer to new operators of a purpose built care home in Derbyshire.
More
Practical Completion on Site Acquired by HPC
This is the latest Practical Completion of a care home development on another great site, sourced and acquired by HPC.
More
HPC assist Aspire LPP in Kent care home planning appeal
Hearing evidence from a Director of HPC has assisted a longstanding client in gaining consent for development in Whitstable.
More
Unanimous Committee approval for new Deal care home development
HPC has been instrumental in supporting Boutique Care Homes in their continued expansion
More
Care Home For Sale - North Yorkshire
Established residential home with day care centre and registered manager in place
More
Integrated Retirement Community Successful at Appeal
HPC provide Expert Witness Evidence on behalf of Inspired Villages
More
Successful Outcome in Wetherby Planning Appeal
HPC provides an assessment of Care Home Need in support of new development
More
Complex Sale of Former Care Home Site Completed by HPC
This challenging project demonstrates the benefit of our experience in the sector and commitment to getting the job done.
More
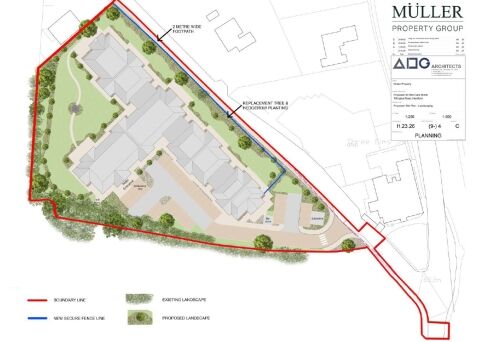
New Care Facility Gains Planning Consent in Kidderminster
HPC advises Muller Property Group in respect of the level of need for Care Home Development
More
HPC Acts in Retirement Sale of North Yorkshire Care Home
HPC has acted for the vendors in the sale of Meadow Lodge Care Home in Kellington, North Yorkshire.
More
Significant Care Home Need in Wiltshire
HPC advises Aspire LPP on Melksham Planning Application
More
Sale of Purpose Built London Care Home Completes
HPC has represented a major provider in the sale of a purpose built care home inside the M25
More
HPC Attends Official Opening of New Harrogate Care Home
Having acquired the site on behalf of Angela Swift Developments, the impressive new home is now operational
More
Future proofing care home provision in the London Borough of Merton
HPC assists Care UK in accommodation upgrade
More
Planning success in Woodley Green, Berkshire
Boutique Care Homes granted Consent with HPC support
More